- TOOL KITS
- A. The NEXT Step
- B. Promoting Independence
- C. Phone Apps
- D. Return to Work
- E. Motivational Interviewing
- F. Paediatric Brain Injury Rehabilitation Resources
- a) Introduction
- 0. Introduction
- 1. Working together promoting independence
- 2 . Using this kit
- b) Issues, goals, action
- 3. Identifying issues W
- 4. Setting goals W
- 5. Making goals happen W
- 6. Monitoring progress W
- c) Strategies Myself and my relationships
- 7. My behaviour's changed W
- 8. Thinking
- 9. Relationships W
- 10.Conversations
- Managing memory, money and time
- 11. Remembering information and messages
- 12. Finances and handling money W
- 13. Managing time W
- Household tasks
- 14. Food and shopping W
- 15. Food and meals W
- 16. House keeping
- 17. Laundry
- Getting around
- 18. Public transport W
- 19. Accessing the community
- Life tasks
- 20. Self care
- 21. Fitness
- 22. Leisure
- 23. Employment
- 24. Continue learning
- 25. Health and well-being
- Emergencies
- 26. Emergencies
7. My behaviour's changed
- 7.0
My behaviour's changed
processes - 7.1 W
Irritability
and anger - 7.2
Changes in
sleep patterns - 7.3
Fatigue and
tiredness - 7.4. W
Increased
anxiety - 7.5.
Problems
adjusting
My behaviour has changed what do I do?
After a head injury you may notice changes in your personality thoughts and/ or emotions. Even though no-one experiences exactly the same set of problems, there are some changes that occur more frequently than others. These can include:
 1.1 Increased irritability and decreased anger control
1.1 Increased irritability and decreased anger control
1.2 Changes in sleep patterns
1.3 Increased fatigue and tiredness
1.4 Changed emotions
1.5 Increased anxiety
1.6 Problems adjusting to the physical or life changes you are experiencing.
All of these problems are discussed in more including tips on ways that you might be able to deal with them.
I have become increasingly irritated and get angry more easily.
Problems with irritability and anger are very common after a head injury. The extent of these problems can vary from person to person, but it can include anything from feeling increasingly frustrated over small/ simple things to having extremely violent verbal and physical outbursts.
In order to control your irritability and anger, it is helpful to identify what triggers you off. Everyone has a unique set of triggers, these are the things that make you feel angry or frustrated and may include loud noises, people speaking abruptly to you, traffic jams, and being kept waiting. You may find your likelihood of being irritable is greater in the morning or the afternoon or evening.
If you know what makes you angry then you can start predicting when you may get angry and take steps to avoid it.
Practical exercise

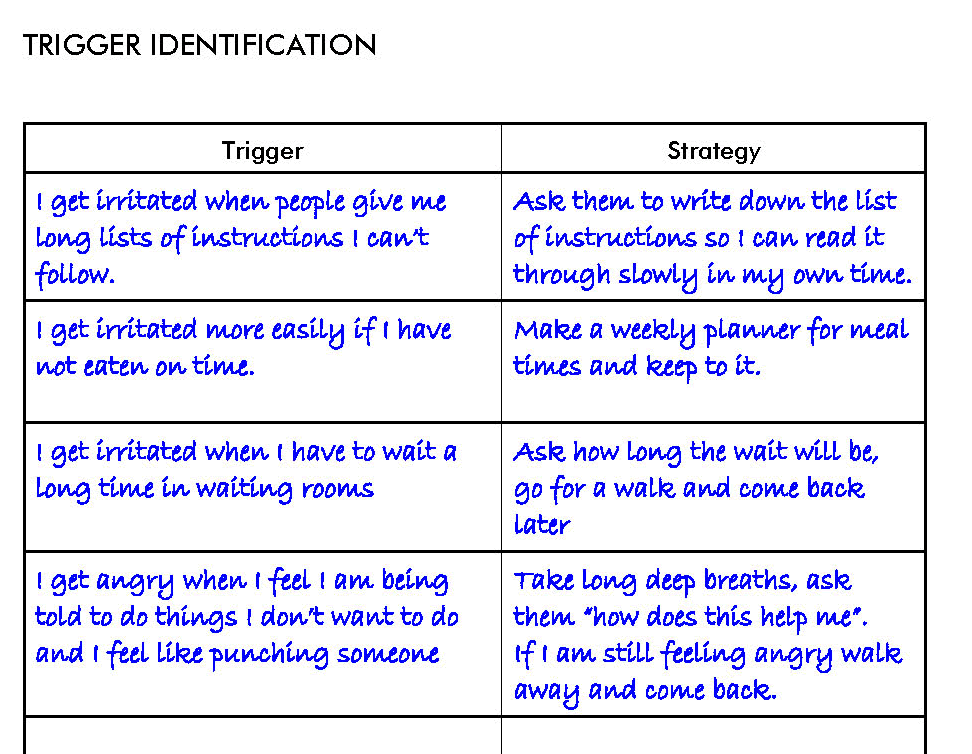
On Worksheet 3 write down triggers you can identify which you think increase your irritability and anger. If you live or work with others, ask them if they notice anything that increases your tendency to become angry or irritable. If you can recognise your individual triggers you have more chance of being able to decrease your irritability and prevent yourself becoming angry. Also on Worksheet 3 write down if there are any strategies you use to prevent yourself from becoming irritable or angry. These provide a starting point from which you can add more strategies. Here is an example.
Helpful hints
The steps you can try and take to calm yourself down, when you feel the anger rise up inside are:
- Tell yourself to 'keep calm' and 'in control', or develop a short sentence that you can repeat to yourself when trying to keep yourself calm. Some examples that people use are, "It will be ok. .. just stay calm", "keep your cool, it's not worth it", and "it will be alright".
- Walk away. It's always better to walk away than to hurt or hit someone.
- Control your breathing. Breathing fast just increases your oxygen level and makes you feel more out of control. To help
stay calm, take long slow deep breaths (try and pause between breaths for two seconds).
- Try and distract yourself by doing something else or by using up energy. For example you can go for a walk, do the gardening, take a bath etc.
- Avoid using alcohol or other drugs when angry, as this sometimes makes it worse. You don't need to complicate your problems by adding an alcohol or drug addiction to them.
Strategies for action
If your goal was to decrease your irritability or aggression, or to keep it under control in certain situations, the following steps may be useful.
- Identify what your triggers are.
- Identify strategies you may already use.
- Identify one of these triggers to work on. You may decide to try one of the strategies listed above or one of your own.
- Write on your goal sheet what trigger you are going to work on and what strategy you are going to try and use to control it.
- Think of a situation where you came across a trigger situation and where you can see that you kept your cool.
- Write down when you plan to review this strategy. It may be one week or three.
- Identify if you think you may need some help to follow these steps. Help may be from a family member, case manager or from a clinical psychologist.
Remember it is difficult to work on everything at once. Take it one at a time!
Franks Experience
Frank had his brain injury nine years ago. He lived with a family friend in the community: The house they shared was more like a duplex, with Frank having his own area where he looked after himself. Frank worked with Community Options workers to perform community activities such as shopping.
Frank's flatmate would drink a lot and would encourage Frank to drink also. Frank kept a journal as he realised he was becoming increasingly angry and he wasn't sure why.
Staff at the Brain Injury Rehabilitation Unit suggested it might be a combination of the alcohol and the situation. Frank thought he would find out. After keeping the journal Frank found that it was the case.
He found that when he had been drinking he became angry if he was asked to do something he didn't want to. He also found that he became angry when people gave him long lists of instructions or too much information because he wasn't able to follow what he was meant to do. This enabled Frank to see how his drinking was contributing to his anger problem and also identified a new goal being able to manage information overload!
My sleep pattern has changed since my injury. What can I do?
Often sleep patterns can alter after a head injury This can mean that you either sleep more or less than you used to, or that you sleep the same but now have a disturbed sleep with frequent waking. Any disturbance of sleep should be brought to the attention of your doctor, as there may be a medical reason or you may need medication.
Helpful hints
Things to try to help you sleep are:
- Try to keep a regular routine of sleep hours, even though you may no longer be working or studying. Continue to rise early and don't stay up late at night or until all hours of the morning.
- Decrease your amount of caffeine drinks and try not to drink any caffeine drinks two hours before going to sleep.
- Have a hot bath before bed.
- Don't attempt any new mental or physical task two hours before bed.
- Try to keep the bedroom purely for sleep purposes. Avoid watching TV in bed, listening to music or reading in bed, as this can often stimulate you mentally and keep you awake.
- If you cannot fall asleep within an hour of going to bed, it is often useful to get out of bed and return when you become tired.
- Keep yourself physically active throughout the day: Become involved in sports, walk or keep busy around the house, cleaning inside or doing gardening. Expend some energy - don't just sit and watch television. If you don't work your body, it won't need to be rested!
Strategies for action
If your goal was to try and increase or decrease your sleep patterns, try the following steps to achieve your goal.
1. Keep a journal for a week to write down what you have done each day. You can write this information in your diary if it is big enough. Make sure you write down what you were doing before bed and the times you woke and went to sleep. See Section 13 Managing time to see how you can keep a journal.
2. The following day write down if you slept well or if it was broken sleep. Write down if you had to get up during the night or if you woke up feeling tired or refreshed.
3. Keep this journal for at least one week, try two. Then sit down and review this information you have gathered about your sleep patterns. Look to see what you were doing on the days before the nights when you slept well. Compare this with what you were doing the days before the nights when you slept badly. If you are finding it difficult to see any patterns, you may need to seek help from a family member, friend, support worker or a staff member from the Brain Injury Rehabilitation Program.
4. If you see there was a pattern then try and do what you were doing on the days of the good sleep. If there was no pattern, then try some of the helpful hints mentioned above. Make sure you write which ones you are trying on your goal sheet. Try one or two of them at a time, then you will be able to work out which ones are helping and which ones aren't.
5. Continue to keep a journal as you try each of these strategies to see if your sleep patterns change. Review your journal each fortnight to see if there are any patterns. Keep your goal sheet up to date to see what strategies you have and haven't tried.
6. If you find you have not been able to modify your sleep patterns with these strategies, it may be necessary for you to see your doctor or clinical psychologist. Take the information you have been keeping in your journal and show them. They may see a pattern you have missed or may recommend some medication that will improve your sleeping.
Jacqui's experience
Jacqui lived in her own home. She stated she was not able to sleep and that she stayed awake till late and then fell asleep in her lounge chair. Jacqui stated she couldn't sleep in her bed as she felt like she stopped breathing. Jacqui had cause to come into the transitional living unit, which is part of the Brain Injury Rehabilitation Unit. While there, her sleeping continued to be a problem. Staff worked with Jacqui to record her sleeping patterns and what she had participated in the day before. At the end of a week, the staff provided Jacqui with feedback. They found she did not participate in the program during the day and instead spent most of her time sitting and watching television. They also found she slept for approximately two hours every afternoon, sitting in the lounge chair and then stayed up late to watch television programs that came on at midnight or the early hours of the morning.
When provided with this feedback, Jacqui and the staff identified some possible strategies to enable her to resume a better sleeping pattern. These included videoing the late night shows to watch the next day, participating in the daily program so she expended some energy and did not have the opportunity to sleep for two hours each afternoon, and trialing a hospital bed that was able to be semi¬reclined so she could sleep in her bed and not in the lounge chair.
Jacqui trialed these strategies and the staff continued to keep a log of her sleeping patterns. The journal showed that when Jacqui participated in the program, did not sleep in the afternoon, slept in the hospital bed and videoed the evening shows, she woke in the morning with more energy, was in a better mood, had less pain in her back and legs and returned to a fairly normal sleeping pattern.
I always seem fatigued and get tired more easily. If I go out in the morning by the time I get home in the afternoon I feel really tired and just can't find the energy to do anything else.
Fatigue is very common after a head injury and you shouldn't label yourself as lazy if you feel this way: Following a traumatic brain injury people can feel very tired, no matter how much or how little sleep they have had the night before. Often these feelings of tiredness are worse in the afternoon or after you have been involved in an activity that has required a lot of effort or concentration. The extent of tiredness will depend on what sort of injury you have sustained and how much rehabilitation you are going through. Sometimes it gets better with time, but sometimes it does not and you have to restructure your day around it.
Helpful hints
If you feel tired:
- Organise to take short breaks during the day.
- Don't try and do too much at one time.
- Break up the task or chore into small manageable bits and take breaks between doing them. Try to keep tasks short so they can be done quickly. If you know an activity is going to take you a long time to complete then try to take regular breaks.
- Don't label yourself as lazy.
- Try and do things when you are at your best and freshest (usually mornings). This may be when you feel alert and energetic.
- Understand that the harder you have to work at something, either physically or mentally, the quicker you will become tired. So expect it and plan for it. Complete more difficult tasks first leaving the easier tasks until later on. Avoid beginning any new activity later in the afternoon when you are likely to be feeling tired.
Plan to do your activities throughout the day, and then balance these throughout the week.
Strategies for action
If you are experiencing an increase in fatigue and tiredness try these following strategies.
1. For one week write down everything you do during the day. Write down the activity, where it was done, transport you used if you had to leave home and how long the activity took to complete. Write beside each part of the activity if you felt tired, all right or good after you completed that part. Write this information on a timetable or keep a journal (See Section 13 Managing Your Time).
2. After one week look at what activities you did, when you did them and how you felt after them. Some questions to ask yourself include:
- Did I spread my activities out over the day?
- Did I spread my activities out over the week?
- Did I take regular breaks during the activity and rest after?
- Did I leave myself enough time or was I rushed to complete the activity?
- What activities made me most tired?
- What part of the day did I feel most tired and what part of the day did I give myself most to do?
3. After answering these questions, the next step is to plan your time. This can help decrease your fatigue and tiredness. You can develop a weekly timetable. This enables you to plan activities throughout the day and then throughout the week. Now you know what activities make you most tired, you can plan to have rests during and after them. See Section 13 Managing Your Time, to see how to complete a weekly timetable.
Brian's experience
Brian is twenty years old. He found he became increasingly tired and wasn't able to finish off any activities he started, whether they were household activities or hobbies and interests. To try and work out why he decided to keep a weekly timetable to see how he spent his time. He did this for one week. After the week he looked at his timetable and noticed to his surprise he was doing all of his household and leisure activities in three days. He also saw it was these three days that he felt most tired. He noticed it took him the following two days to recover from the first three days of activity. He also saw it took him a lot longer in reality to complete activities, which meant he felt he was rushed because he hadn't left enough time. Brian decided he would try and structure his time better using a weekly timetable. Brian planned to complete all the activities he had tried to complete in three days over seven. He allowed more time to complete these activities and took rest breaks after he had completed each activity. The following is an example of Brian's timetable before and after he tried to balance his week. Brian stated he had more energy to do what he wanted - go out with friends and hobbies - once he had spread out his activities over the week. He said he didn't feel as tired and had energy to watch television at night.
The following Worksheet includes with it Brian's first and second weekly timetables and Gemma's weekly timetable.
See Section 13 for more hlep with using weekly timetables.
It seems as though all my emotions have changed or are mixed up. Why?
If you find that you are more emotional than you were, there can be a couple of reasons for this. Firstly, it could be that the part of your brain that controls your emotions has been damaged. This means that you may laugh and/or cry extremely easily and at things you wouldn't have previously; Secondly, you may be experiencing a depressed mood. If you think you are depressed, tell your doctor, as you may need medication and might be helped by some counseling.
Practical exercise

On Worksheet 3 write down triggers you can identify which you think increase your anxiety.
Strategies for action
If you are experiencing changes in your emotions:
1. Think about what triggers you to cry or laugh or feel depressed. Write these down. You can keep a journal over a week-long period to see what triggered you during this time. See Section 13 Managing Your Time to see how to keep a journal.
2. At the end of the week ask others with whom you live or are friends, if they have noticed anything that can cause your emotions to change. Write these down also.
3. Once you are more aware of when your emotions may change you can have a plan of action. This may be leaving the situation, telling a person you're chatting with you'd like to change the subject or thinking about something positive.
4. On your goal sheet write down the trigger you are working on and the situation in which you want to control that trigger. Also write down what strategy you are trying to use.
Peter's experience
Peter is forty years old. He was hit by a motor vehicle when riding his bicycle. He had a brain injury and broke nearly all the bones in his body. He found that as he was trying to get on with his life after leaving hospital he was becoming teary and upset because he couldn't do everything as he used to. Peter loved sport, was always running or riding and worked hard enjoying the challenge. Peter decided he wanted to find out what was triggering his teariness and depression. Peter kept a journal and recorded when he became upset, what he was doing at the time or what he was thinking about. When he looked at the different journal entries a week later he found that he became upset when he was faced with something he was able to do before but had difficulty with, or couldn't do, now. Peter decided that instead of pondering what he now couldn't do, he would do similar activities to achieve the same purpose. Peter took up swimming to improve his fitness and while he had returned to work part-time decided he would find another interest for the other days. Peter spent time with a psychiatrist who prescribed him some antidepressants and Peter worked on strategies with the clinical psychologist to manage the depression.
I have become increasingly anxious about all kinds of things. Why?
Feelings of anxiety can come in many forms. It can range from sweating and your heart pounding, to an avoidance of a place or situation, to a general feeling of restlessness. There are too many reasons for feeling anxious to list them all here.
Therefore it's important that you try and determine what is making you feel anxious and to talk to someone about helping you try and control it.
Helpful hints
Things to try to reduce your anxiety are:
- Control your breathing. Take long slow deep breaths with pauses in between them.
- Tell yourself to keep calm.
- Don't let the anxiety take control of your life. Talk to a doctor or psychologist if this is happening.
- Tell your family what is happening and talk about it with them.
- Avoid using alcohol or drugs to help you control your anxiety.
- If your anxiety takes the form of flashbacks or nightmares, tell your doctor.
Peter's experience
Peter became very anxious about being around lots of people, in crowds or in confined places after he had his brain injury. For a long time Peter did not go to places where he thought there might be crowds or confined places. One day he was asked to attend a conference for his work in the city. Peter had to catch the train in peak hour to be at the conference on time. Peter stated he decided he had to face his fears. He reported practicing what he would do in each situation before he actually left to catch the train.
When Peter went on the train, he stated that he repeated to himself to stay calm, and focused on taking long slow breaths. Peter also left earlier than he had to so he could rest and take some time to gather himself before the conference started. Peter rewarded himself with a cappuccino when he made it to the conference venue.
Peter now uses public transport independently. He stated he still gets anxious but is working on strategies to relieve this anxiety with the clinical psychologist at the Brain Injury Rehabilitation Unit.

